by M | Jul 11, 2020 | News |
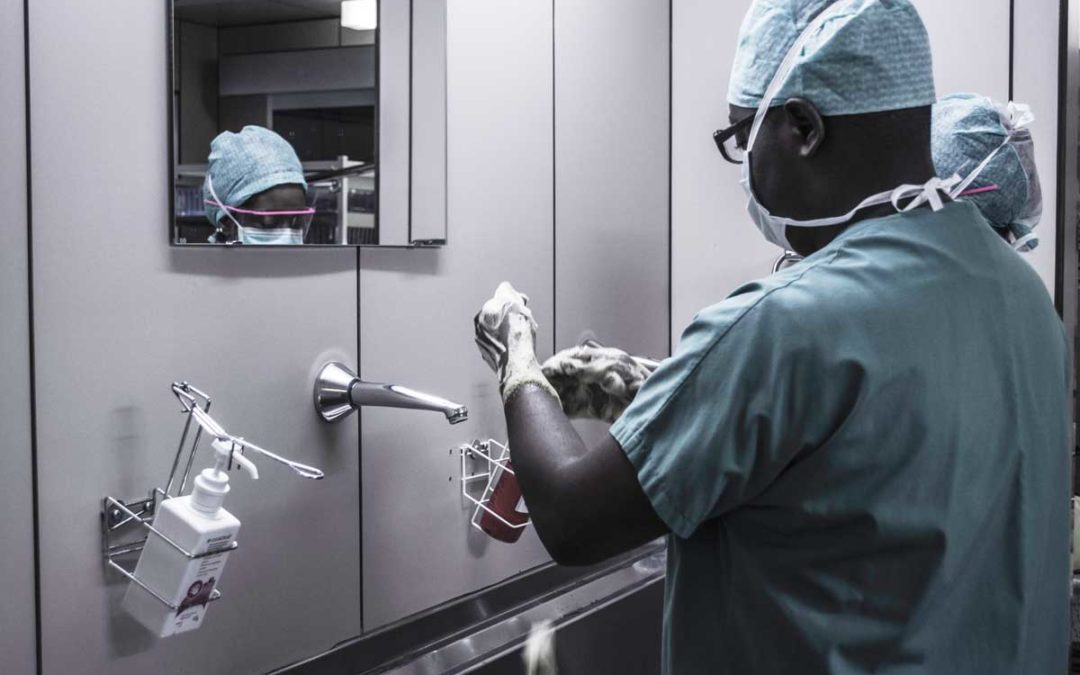
More than half of all accountable care organizations (ACOs) deliver home health care to their patients, while an additional 17% have new home visit programs in the works.
That’s according to a recent survey of National Association of ACOs (NAACOS) members, conducted in conjunction with the Institute for Accountable Care (IAC) and West Health Institute. Washington, D.C.-based NAACOS is an industry advocacy group representing hundreds of ACOs, which cover an estimated 23 million patients who have Medicare, commercial insurance and Medicaid.
The survey findings should come as welcome news to home-based care providers, who have long tried — and largely failed — to build partnerships with ACOs. Home health providers have argued that they can help improve patient outcomes, but ACOs have often undervalued that ability.
The coronavirus is only likely to help prove home-based care’s worth, according to Rob Mechanic, senior fellow at the Heller School of Social Policy Management at Brandeis University and executive director of IAC, a Washington, D.C.-based research organization founded by NAACOS.
“Since COVID, … there are some [ACOs] that are frankly growing their [home-based care] programs, because they’re concerned that patients are not seeking treatment when they have serious problems,” Mechanic told Home Health Care News. “I think home-based care is tailor-made for ACOs.”
Despite Mechanic’s COVID-19 predictions, the aforementioned survey was conducted in a pre-coronavirus world. It ran from the end of September 2019 through the start of January 2020, polling ACOs on their home-based care practices.
A total of 163 ACOs were surveyed, with the large majority of respondents being participants in the Medicare Shared Savings Program. A few were Next Generation ACO program participants.
Of the respondents, 26% said they have a home visit program, while 25% conduct home visits but don’t have a formal program. Additionally, another 17% have a home-visit program in the works.
Only 32% of respondents said they had no plans to start a home-visit program.
The full results of the study have yet to be released because the findings have been submitted to a peer-reviewed journal. However, Mechanic said the results reflect the growing interest in home-based care delivery by ACO programs.
“It didn’t surprise me at all because, frankly, this is something that makes a lot of sense for ACOs,” he said. “ACOs ultimately are judged against a global budget, a total home health care budget. So ACOs can afford to invest in non-billable, non-revenue producing activities that will lower home health care spending.”
The main reason respondents reported having a home-visit program was to deliver primary care. Other popular reasons for having a home-visit program were to support care coordination efforts and transitions from in-patient settings to the home.
A smaller percentage of respondents said they have a home-visit program to better address social determinants of health. Some also said their home-visit programs were part of a hospital-at-home model.
While a growing number of ACOs seem to be coming around on home-based care, that doesn’t automatically equate to shared savings for home health care agencies.
There’s a lot of diversity in how programs are delivering home-based care, Mechanic said, but generally even when in-home health care companies have been involved with ACOs, they’re still left out of shared savings ACOs generate. Instead, the arrangements are usually fee-for-service.
Mechanic is hopeful those relationships will evolve in the future.
“I would like to see, over time, more [ACO] partnerships with different kinds of groups,” he said. “Both ACOs and home health care agencies have to come to the table with open minds and to be flexible and creative. I think that can lead to partnerships that are good for both of them.”
By Bailey Bryant
Source: Home Health Care News

by M | Jul 9, 2020 | News |
It’s time for policymakers, hospitals and everyone else at the home health care roulette table to bet all their chips on proactive, pre-acute home-based care.
During the coronavirus pandemic, the U.S. health care system has undergone a massive change marked by the skyrocketing use of telehealth technology and the shift away from brick-and-mortar medical appointments. In fact, from April 2019 to April 2020, telehealth claim lines have increased by more than 8,300% nationally, according to FAIR Health data.
For the most part, though, traditional home-based care has felt like a secondary priority over the past few months, with home health providers and home health care agencies largely overshadowed by telehealth trends, hospital capacity concerns and the general state of nursing homes, which continue to be devastated by COVID-19.
“I think that [policymakers] have been very responsive to the needs in the hospital setting,” a Maine home health executive previously told Home Health Care News. “I do not feel that they fully understand the complexity of the patients seen by home health and hospice providers.”
Health care stakeholders may have missed the opportunity to aggressively invest in-home health care during the initial coronavirus spike, but that door is opening wide once again. Or rather, it never really closed.
The country’s rolling seven-day average of daily new COVID-19 cases shattered all previous records on Monday for the 28th day in a row, the Washington Post reported. At the same time, hospitals across the Sun Belt are being overwhelmed by coronavirus patients, with Arizona reaching 89% capacity for intensive care unit beds and California, Georgia, North Carolina, Texas and a handful of additional states experiencing unprecedented hospitalization numbers.
The new coronavirus spikes in the South and West aren’t part of a different, second COVID-19 wave. They’re continuations of the first wave that was never properly addressed.
Overall, the U.S. death toll linked to the coronavirus hit 130,000 this week, statistics from Johns Hopkins University show. The number of total infections is approaching 3 million.
With those numbers in mind, Dr. Anthony Fauci, the head of the National Institute of Allergy and Infectious Diseases and a leading member of the Trump administration’s coronavirus task force, is calling for urgent action.
“It’s a serious situation that we have to address immediately,” Fauci said during an online interview Monday with Dr. Francis Collins, who leads the National Institutes of Health as its director.
As part of the nation’s renewed response to the coronavirus, home health and home care need to now be front and center. Fortunately, there are several readily available actions out there that the federal government and other health care players can take to support all shapes and sizes of in-home care providers.
When it comes to home health care agencies, in particular, the U.S. Centers for Medicare & Medicaid Services (CMS) can start by reopening its advanced and accelerated payment programs, allowing operators to focus on patient care and not their finances.
Home health agencies experienced huge financial losses during the early days of the coronavirus due to patients canceling visits and the general suspension of elective surgeries. Cash flow disruptions have somewhat stabilized, but the recent resurgence of COVID-19 cases may retrigger the same anxieties and roadblocks that agencies had to previously overcome.
From March through April, CMS distributed more than $100 billion in advanced and accelerated payments to all Medicare providers. Home health providers received just $1.7 billion of that before CMS shut down the programs — and many home health agencies in emerging hotspots never even had the opportunity to apply for payments, as they’re just now feeling the impact of the coronavirus.
On top of reopening its advanced and accelerated payment programs, CMS should also consider giving home health providers a more robust Medicare rate adjustment. While the National Association for Home Care & Hospice (NAHC) and other industry advocates have called for a 15% rate increase, CMS recently suggested a 2.6% reimbursement bump in its proposed payment rule for 2021.
Many home health providers won’t be able to stay afloat for much longer without additional financial lifelines. In New York alone, home-based care providers expect to lose upwards of $200 million in 2020, according to financial estimates by the Home Care Association of New York State (HCA-NYS).
“These losses have alarming implications for the viability of New York’s home care system and the necessary support it provides for patients,” Roger Noyes, director of communications at HCA-NYS, previously told HHCN.
Meanwhile, when it comes to supporting home care agencies, Congress should start by seriously considering the creation of a fund that helps operators finance hazard pay and other benefits for front-line workers in its next relief package.
It’s an idea that had been floated by House Democrats in their Health and Economic Recovery Omnibus Emergency Solutions (HEROES) Act unveiled in May. Specifically, the House bill included a $200 billion fund for hazard pay for all essential workers.
Interim HealthCare Inc. CEO Jennifer Sheets previously told HHCN she would “love to see” government-supplemented hazard pay for health care workers.
“We need to incentivize people to be on the front line, especially in a pool that’s already prone to high turnover,” she said.
Apart from financial assistance, the Trump administration and FEMA should also organize a personal protective equipment (PPE) push for in-home care providers, similar to what they did for nursing home operators back in April. In-home care agencies have had just as difficult a time securing PPE, if not greater, as they’ve been excluded from most priority lists during the COVID-19 crisis.
Outside of the government, hospitals also need to accelerate the shift toward in-home health care. Many already have, including North Memorial Health Hospital in Minnesota, which recently partnered with whole-person, home health care provider Lifesprk to offer a hospital-at-home model.
“With the outbreak and shortage of personal protective equipment (PPE), one of the just really sad things that all of us have witnessed is when someone goes into the hospital right now and is very sick, their loved ones can’t be there with them,” Dr. Carolyn Ogland, North Memorial’s CMO, previously told HHCN. “This is a way to really help our families and our patients stay together when they are sick.”
If the U.S. health care system acts quickly and invests in home health care, it will emerge from COVID-19 stronger than ever. But the window of opportunity is closing, so stakeholders must act now.
By Robert Holly | July 7, 2020
Source: Home Health Care News

by M | Jul 6, 2020 | News |
When pain radiated from Fred Thomas’ neck down his arm and he couldn’t feel his fingers anymore, he knew it was time to talk to a doctor.
After getting an MRI ordered by his primary-care doctor, the 49-year-old land surveyor had several phone conversations with a Rothman Orthopaedic Institute specialist he’d never met to discuss the problem and treatment options. He was scheduled for a cervical fusion to replace three damaged disks in his spine a couple of weeks later.
“By the time I met him, I felt like I’d been in his office 15 times,” said Thomas, who lives in Wilkes-Barre. “We spoke in person for the first time a few minutes before he operated.”
Months ago, few patients or doctors would have considered surgery without so much as in-person consultation, but the coronavirus pandemic has forced the health care system to embrace telemedicine like never before.
With no other way to see a doctor as the virus shuttered all but the most essential health care service, regulatory hurdles that hamstrung the growth of telemedicine for decades were wiped away: Private insurers, Medicare and Medicaid agreed to pay the same rates for telemedicine visits they would have for in-person appointments. The federal government loosened privacy regulations that had in the past restricted how patients and doctors communicate virtually.
In response, telemedicine visits soared. The approach has been exceedingly popular among patients and doctors, and so universally adopted by health systems that experts say telemedicine is likely here to stay. Not only have health systems proven that telemedicine is an effective and useful tool for treating existing patients, virtual doctors’ visits also present an opportunity for health systems now forced to grapple with the racial inequities highlighted during the pandemic to improve access to care.
“We have this opportunity as the result of a very horrific, virulent disease to re-imaginehealth care service,” said Nicol Turner Lee, a senior fellow at the Center for Technology Innovation at the Brookings Institution.
But maintaining telemedicine will be possible only if providers and insurers are able to agree to fair payment, and if regulators are able to work out security and patient privacy issues.
Exponential growth in telehealth
When the pandemic shut down non-urgent medical services in Philadelphia in March, Penn Medicine quickly equipped nearly 9,000 providers to meet patients by video or phone and now averages 5,000 telemedicine visits a day – a nearly overnight change from a few hundred doctors doing a few hundred visits.
While in-person visits plummeted 90% at Jefferson Health, virtual visits rose from a couple hundred a week in February to 20,000 a week in June. Some of those calls were about coronavirus, but the vast majority were “regular doctors’ visits,” said Judd Hollander, senior vice president for Health Care Service delivery innovation at Jefferson Health.
“Telemedicine grew out as rapidly as it did because people were afraid of COVID and because reimbursement models changed,” said Hollander, an emergency medicine doctor.
Jefferson is now bringing back patients for in-person visits, but Hollander expects that about a third of visits will remain virtual – in part because of how popular the approach is with patients, who score telemedicine “light years ahead” of office visits on patient satisfaction surveys for its convenience.
“They’ve seen the benefit of staying home,” he said.
For Thomas, meeting with his specialist at Rothman Institute by phone or by video eliminated the need for multiple, day-long trips into Philadelphia. That journey would have been especially difficult after his surgery when he was not able to move his neck for several weeks. He had follow-up scans done near his home and spent a few bucks to mail them to Rothman – far less than he would have shelled out on gas and parking.
In the past, telemedicine was considered an option for routine chronic care appointments or quick check-ins. But the pandemic challenged doctors to find ways to perform through video the services they assumed could be accomplished only in person.
“This has broken a lot of long-held principles, like, ‘You can’t do that’ and ‘Change is bad,'” said Bill Hanson, chief medical information officer at Penn Medicine.
At Einstein Healthcare Network’s Moss Rehab, Chris Plastaras, clinical director of musculoskeletal spine and sports rehabilitation medicine, filmed short instructional videos for at-home strength tests.
Even with patients slowly returning to the office, Plastaras often prefers video because he is better able to read facial cues that are crucial to interpreting a patient’s progress – if he saw a patient in person, the patient would be hidden by a face mask.
“If you bring up a treatment option and you see the patient cringe, OK, you don’t want to do that. Or their face brightens, then, OK, we’ll do that more,” he said. “It really is something that’s important as we counsel patients in their treatment options, having that nonverbal feedback.”
Barbara Gilin had spine surgery at the beginning of February, before the pandemic hit. But by the time she was ready for rehabilitation work – typically a hands-on kind of medical appointment – a video visit was her only option.
“I think the biggest surprise to me was how thorough the physical exam could be,” said Gilin, a psychotherapist who lives in Montgomery County and is a patient of Plastaras’.
The insurance hurdle
Even with some stumbling points, such as how to secure prior authorization and get patients needed testing, many health system executives now describe telemedicine as a genie that can’t be put back in its bottle. But the changes that made its widespread adoption possible were intended to be temporary. A permanent change will require more work.
“It was a sensible thing in a pandemic to say just ‘make it happen.’ But it’s not sensible to say ‘there are no rules,'” said Carmel Shachar, executive director of the Petrie-Flom Center for Health Law Policy, Biotechnology, and Bioethics at Harvard Law School.
Federal regulators permitted medical use of Facetime and other popular video chat tools during the pandemic, but these platforms don’t meet federal patient privacy rules.
Private insurance agreements to cover telemedicine during the pandemic are also temporary. But without insurance coverage, virtual visits are impossible.
“This is progress … but if you don’t pay for this we can’t do it and it’s forcing us to go to the older model where people spend 21/2 hours driving in, waiting,” said Alexander Vaccaro, president of the Rothman Institute. “We’re begging the insurers to come up with fair rules.”
Vaccaro said he wants about 30% of Rothman appointments to remain virtual, but doctors have already received notices from most major insurers about their plans to suspend telehealth coverage in the coming months.
The federal Centers for Medicare and Health Care Service has said it is considering making access to telemedicine permanent, which may pave a path for private insurers to follow.
Independence Blue Cross, the largest private insurer in the Philadelphia area, plans to extend its pandemic coverage for telemedicine through the end of the year, said Richard Snyder, the insurer’s chief medical officer. Independence wants to maintain telemedicine coverage. But instead of paying for every test and visit, contracts may instead pay based on how well a patient is cared for.
“I don’t think pre-COVID utilization of telemedicine was in any way optimal,” Snyder said, but neither is it appropriate for every type of visit.
Shifting some appointments to virtual visits could ease strain on doctors’ offices, which are working through a backlog of missed appointments slowly to maintain social distancing. At the same time, hospitals could miss out on revenue if they can’t charge a facility fee.
“We have to start thinking, going forward, what is the right mix of care so we can take care of everyone – and remain financially solvent,” Hollander said.
Opportunities and challenges
The stakes for how telemedicine becomes a permanent fixture also are high because it presents an opportunity to address long-standing inequities in health care service.
“Telemedicine can be an equalizer in the sense that it allows greater distribution of the good stuff medicine has to offer across geography and socioeconomic levels,” said Hanson, of Penn.
Virtual visits may be more accessible for people who lack transportation, can’t take off work, or don’t have child care – barriers that disproportionately affect low-income communities.
Already, Hanson said, Penn has noticed that some patients with chronic health problems have been better able to keep up with their needs through telemedicine than with traditional office visits.
But it can also create new challenges, in particular for people for whom English is their second language or who do not have Internet access.
At Philadelphia’s Strawberry Mansion Health Care Service, the primary-care provider for families in a particularly low-income neighborhood, virtual visits could be helpful, said Tanya Malone, the city-run health center’s clinical director. But many patients aren’t connected to the Internet or don’t have phones with video capabilities. That is a barrier, Malone said, that must be addressed.
“Most of our patients, we are their primary-care physician, we are their home base,” Malone said. “I’m sure we’ll come up with some kind of plan. … This is going to be the future of medicine.”
By SARAH GANTZ | July 06, 2020 04:00 AM
Source: The State

by M | Jul 4, 2020 | News |
Caring for older adults was already expensive, emotionally taxing and logistically difficult — and the coronavirus is only making it worse.
Why it matters: People older than 65 have the highest risk of dying from the virus, and outbreaks have been rampant in long-term care facilities. That is creating anxiety for seniors and their families.
The big picture: Most seniors will need at least some long-term care, but the coronavirus has added even more complications to the tough decisions about how to obtain it.
- Assisted-living and independent-living facilities cost an average of at least $4,000 a month, almost always paid out of pocket.
- Nursing homes are generally more affordable, but people often have to burn through their savings, pensions and other assets on their way there.
- Nursing homes also are cramped, understaffed and have poor track records with infection control to begin with — and they’ve been hotbeds for the spread of the coronavirus.
- Home care is another option. If a professional worker isn’t available, the task often depends on the charity of a friend or relative, and that’s a dicier proposition when those friends or relatives could be carrying the virus — or unemployed, caring for children or otherwise just not able to help.
Where it stands: The pandemic has severely hindered operations across the industry.
- Senior housing operators have limited tours of rooms and communities to prospective residents and one family member, or they are only providing virtual tours. That limited recruitment, combined with widespread outbreaks and lockdowns, has led to fewer people moving in.
- The federal government is starting to ease some restrictions at nursing homes, but is saying they “should be among the last to reopen within the community.”
Controlling outbreaks depends on facilities stocking up equipment for employees and conducting widespread testing — things the industry hasn’t exactly been heralded for.
Between the lines: Seniors who want to avoid the virus-related risks could try to stay and get care at their homes, which more people have done in recent years. Adult children also may try to move their parents closer to their homes.
- “But not all parents want to do that,” said Toby Edelman, a senior policy attorney with the Center for Medicare Advocacy.
- Home health aides can also be hard to find. Despite the demand, the job pays poverty-level wages.
The bottom line: “Especially with the way [the coronavirus] has spread at these facilities, there’s going to be a fear until there’s trust that the risks are sufficiently low,” said Carri Chan, a health care business professor at Columbia University.
By Bob Herman | May 26, 2020
Source: AXIOS
by M | Jul 3, 2020 | News |
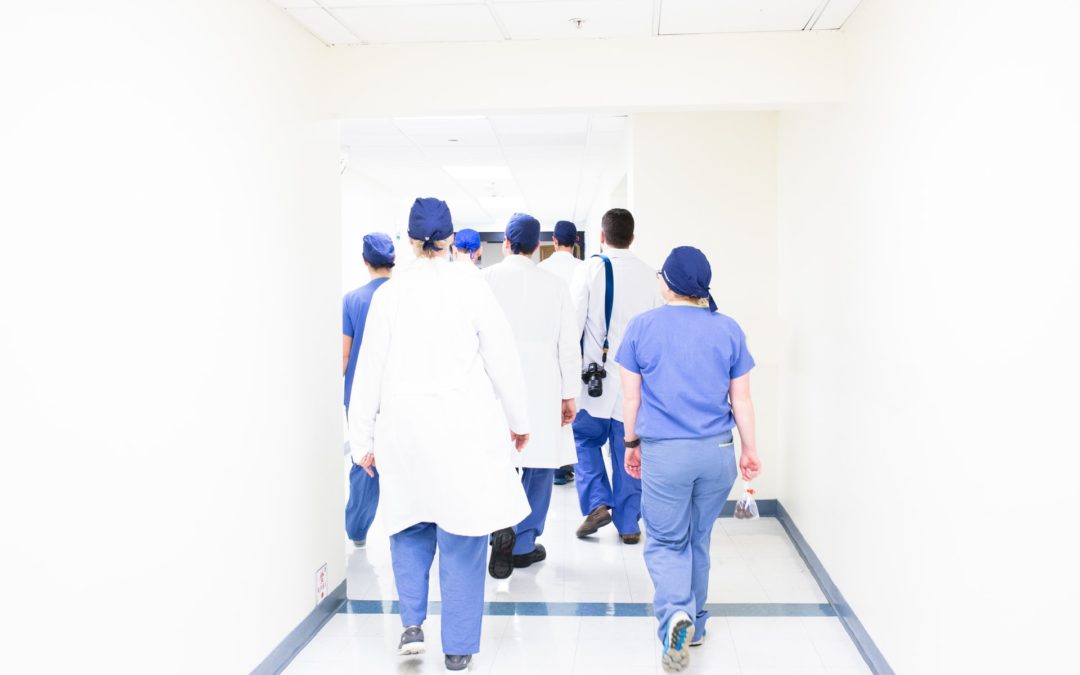
Nursing homes have been the epicenter of the coronavirus outbreak, prompting more urgent discussions about alternative housing situations for elderly Americans.
Why it matters: Deaths in nursing homes and residential care facilities account for 45% of COVID-19 related deaths, per the Foundation for Research on Equal Opportunity — but there are few other viable housing options for seniors.
- COVID-19 illness severity and mortality rates have been highest among older adults — a fast-growing segment of the U.S. population as Baby Boomers age.
The alternatives that are available are getting a closer look. Here are the ones that are growing in popularity:
“Granny flats“ — or small units built in backyards, above garages or in basements — are seeing the biggest surge in interest, experts say, because they are often easiest to tack onto existing structures and get less resistance from the NIMBY crowd.
- They allow aging parents and grandparents to live near caregivers and can offset living costs for homeowners.
- Some cities are trying to make them easier to build. Most recently, the Austin city council in April directed staff to find funding for low-cost loans and streamlining the permitting process in a push to increase the use of secondary units (or accessory dwelling units) in the city.
Multigenerational living has increased over the past decade, with 9.3 million people over 65 living with grown children or grandchildren in 2017.
- As the trend picks up, housing design will have to follow suit, according to Jennifer Molinsky, senior researcher at the Joint Center and lecturer in urban planning and design at Harvard. That means houses built with two master suites, an in-law suite or other flexible space.
- In a recent AARP survey, 52% said the benefits of living in an intergenerational home outweigh the disadvantages and risks posed by COVID-19. But ages 50-59 are most likely to see those benefits, with older age brackets more heavily weighing the downsides.
Co-living — or living with roommates and sharing common areas a la “The Golden Girls” — is still relatively small among the the 65 and older camp, but the rise of services that match older roommates like Nesterly and SilverNest has boosted interest.
- With “homesharing,” older adults with extra room can take on a tenant to help pay bills and decrease loneliness, allowing them to stay in their house for years longer.
- “It’s logical to conclude that with extended periods of isolation that interest could increase,” said Danielle Arigoni, Director of AARP Livable Communities. “But on the flip side, it may be that people are more afraid of having a roommate right now.”
By the numbers: The number of households aged 75-79 will rise 49% between 2018 and 2028, while those age 80 and over will account for 12% of all households by 2038, per Harvard’s Joint Center for Housing Studies.
- More than half of individuals in this age range live alone.
- And in many metro areas, more than a third of older households are cost-burdened, meaning they pay more than 30% of their income for housing.
The big picture: Most communities do not have the housing that will be needed as their residents age.
- Many older adults either can’t afford to downsize as the nation’s housing stock has grown bigger and more expensive, or they don’t have enough savings or retirement funds to keep paying a mortgage or the rent for pricey long-term care centers.
- A growing number of older adults live in low-density areas filled mostly with single-family homes and requiring cars to get around. That’s problematic both for seniors looking to downsize and for those who can no longer drive themselves.
- “To the extent people want to stay in communities where they’ve been living, we’ll absolutely need more housing options, such as apartments and denser more walkable solutions that are lower cost,” Molinsky said
Between the lines: Even with new options for semi-independent living situations and increased concerns around nursing homes, service-rich residential housing that provides meals, transportation and medical care will still play a large role as we live longer and require more around-the-clock attention.
By Kim Hart | Jul 2, 2020
Source: AXIOS

by M | Jul 1, 2020 | News |
In the span of less than four months, COVID-19 has killed around one in every 40 nursing home residents in the United States—some 32,000 people as of May 31, according to federal data. More than 600 nursing facility staff members have also died from the disease.
SARS-CoV-2, the virus that causes COVID-19, is especially lethal to older people, and it has spread quickly in the close quarters of many facilities. In New York City, some nursing homes were forced to convert refrigerator trucks into temporary morgues to handle the surge of corpses. At one home in New Jersey, as bodies piled up in a small morgue, staff briefly resorted to storing a body in a shed.
Today, many nursing homes across the country remain on lockdown, and the devastation, experts and advocates say, underscores longstanding issues with a system that, even in normal times, struggles with understaffing, poor infection control, and neglect. Now, the COVID-19 pandemic has energized calls for a more drastic solution: closing nursing facilities altogether.
“Why do we have these facilities where people are not receiving proper care?” said Susan Dooha, the executive director of the Center for Independence of the Disabled, New York, which advocates for people with disabilities, including those that result from aging. “Maybe we don’t need them.”
That sentiment echoes the latest foray in a much larger, longer-running push for deinstitutionalization. The effort has long sought—with some success—to expand at-home or in-community care options for disabled people in need of long-term care. But as COVID-19 has ravaged elder-care facilities in the US and around the globe, advocates are now increasingly asking whether the reflex toward institutionalized care for seniors is due for a drastic rethinking, too.
“There’s been a very interesting divide between disability rights groups and, for want of a better expression, elder rights groups, because the elder rights groups seem to be okay with some form of institutionalization,” said Gerard Quinn, an Irish legal scholar who helped draft a landmark United Nations convention on disability rights, and who has recently argued for the gradual abolition of nursing homes.
But since COVID-19, Quinn added, “a lot of the elders rights groups now are turning completely around and beginning to understand the importance of living well in the community with adequate supports.”
In the US, such ambitions have run up against the challenges of remaking the nursing home industry, largely funded by billions of dollars in federal Medicare and Medicaid payouts. That industry is tasked with providing specialized medical care to some of the most vulnerable people in the nation, and the need for such care is only expected to grow as the Baby Boomer generation ages. And, in light of the challenge of providing 24-hour and rehabilitative care, not all experts are convinced that a complete move away from institutions is possible.
“Why do we have these facilities where people are not receiving proper care? Maybe we don’t need them.”
“I think at the end of the day, you might not really be able to,” said Anna Rahman, a gerontology researcher at the University of Southern California. “There are some people who are very, very sick, and their families cannot take care of them.”
Sometimes, Rahman added, “you can’t afford to assign one person—one person, 24/7—to a person who needs help.”
But the stakes of reform, advocates agree, are high—and have only become clearer during the current pandemic. “We have, since COVID began, received a lot of calls from people desperate to leave facilities,” said Dooha. Through calls from residents and staff, she added, her organization has “learned that conditions in facilities are utterly deplorable.” Those conditions, Dooha says, should cause more people to question a system that, in the US alone, houses around 1.3 million people.
Nursing homes became commonplace in the 20th century, enabled by twin shifts in American life: government aid for the elderly, and medicine that allowed more people to reach an age where they could actually use it. Such facilities began multiplying shortly after the passage of the Social Security Act in the 1930s, and they expanded with the introduction of federal- and state-run health programs like Medicare and Medicaid in the 1960s.
These homes fit into a larger category of institutions sometimes referred to as congregate care settings. Often used as an umbrella term, congregate care settings include psychiatric hospitals, group homes, and assisted living facilities. Nursing homes are distinguished by their capacity to provide skilled nursing care and, typically, 24-hour support for residents. (While the majority of nursing home residents are seniors, younger people with disabilities can end up there, too. Around one in seven long-term nursing home residents is under the age of 65.)
For decades, some disability and, to a lesser extent, seniors’ rights activists have fought to end the impulse toward institutionalization, and those efforts have helped build infrastructure to support elderly and disabled people living within the wider community. In the early 2000s, policymakers began doing more to prioritize home care for people who might otherwise have ended up in a facility. Emphasis was placed on supporting patients who could receive care in their own homes, either from family members or home health aides.
“Over the last two decades, there’s been a tremendous change in the long-term services system,” said Robert Applebaum, a professor at the Scripps Gerontology Center at Miami University in Ohio.
“Even in a state like Ohio,” he added, “where the nursing homes were really quite a powerful entity, we’re now serving more older people at home or home-community-based services than we are nursing homes.”
A major 2018 survey from AARP, the aging advocacy organization, reported that close to four-in-five Americans aged 50 and above prefer to age at home. “Most older people are anxious about the prospect of moving into a nursing home,” a recent analysis of studies in high-income countries reported, and studies consistently show high rates of depression in facilities.
Congress has allowed states to divert Medicaid funds for care outside institutions since 1981. But the move toward deinstitutionalization, critics says, has been too modest. One reason: Medicaid policies push older people into facilities, even when they would prefer to live at home. Medicaid “has an institutional bias,” said Rhonda Richards, a senior legislative representative for AARP. “It covers nursing home care for people who are eligible, but coverage for home and community-based services is much more optional and discretionary.” Policies vary by state, she said, and not everybody who meets the eligibility criteria for receiving care at home will actually receive those services.
This remains true despite arguments that institutional care is more expensive — and even though many nursing home facilities suffer from what critics say is a well-documented history of problems. Staff turnover rates are, for example, famously high. Staff receive low wages and may be unable to report problems without risking their jobs. In turn, residents may be afraid to reveal abuse or mistreatment, for fear of retribution from staff. Some facilities house three or four residents in a single room.
For years before COVID-19, researchers have warned that norovirus, influenza, and other infections can spread rapidly in nursing facilities. Those risks have increased in recent years, as nursing homes take in more short-term residents who are getting rehabilitation after hospital visits, and who potentially bring infections into the building with them, said Lona Mody, who runs the Infection Prevention in Aging Research Group at the University of Michigan Medical School. In addition, Mody said, “staff members’ compliance to hand hygiene in the past has been not good.”
Advocates say that these and other problems have only intensified as large companies began buying and consolidating nursing home franchises. Around 70 percent of nursing homes in the United States are under for-profit ownership, and, since the 2000s, private equity firms have purchased many facilities, hoping to cut costs and increase profits. One recent analysis, published by the New York University Stern School of Business, found “robust evidence” that private equity buyouts were linked to “declines in patient health and compliance with care standards.”
Then came the COVID-19 pandemic.
The first major outbreak in the US took place at the Life Care Center of Kirkland, a suburban Seattle nursing home owned by Life Care Centers of America, a company with more than 200 facilities around the country. The virus killed 37 people linked to the home in a matter of weeks.
In the months that followed, hundreds of nursing homes have seen major outbreaks, with the toll falling particularly heavily on facilities with larger populations of people of color, according to a New York Times analysis published last month. Meanwhile, many nursing homes and other residential care facilities have struggled to maintain staffing as low-paid workers are asked to risk their lives to offer care to residents, sometimes without adequate personal protective equipment.
In late March, a federal government report found that more than one-third of facilities were violating handwashing protocols. And as the virus overwhelmed many facilities, some family members struggled to get information about their relatives living inside. The issues, advocates say, have extended to other care institutions, such as psychiatric facilities.
In response to criticisms, industry representatives argue that the COVID-19 pandemic’s outsize impact on nursing homes had little to do with the quality of care, and more to do with the challenges of stopping a fast-moving, little-understood virus. “It’s really not an issue of what nursing homes could or couldn’t have done,” said Stephen Hanse, the head of the New York State Health Facilities Association and New York State Center for Assisted Living, a trade organization representing more than 450 facilities. “It’s really a function of what this virus is,” he said, citing initial studies that have found little link between a facility’s quality ratings and its coronavirus impact.
But the scale of suffering during the pandemic has led to calls for change. “We’ve created this system, and now we’re telling all the people who work in it to just make it work. And it doesn’t work,” said Sonya Barsness, a gerontology consultant who works on reforming nursing home culture.
“This pandemic,” she added, “has brought light to the reality that the system is not adequate to support the needs of people as they grow older.”
What a new system may look like is unclear, and some advocates argue that the structural problems that plague nursing homes won’t be solved by increased regulation or funding. “You can’t throw any more money into this institutional model,” said Fiona Whittington-Walsh, a disability studies scholar at Kwantlen Polytechnic University in Canada and the president of the board of directors for Inclusion BC, an organization that has fought the institutionalization of people with developmental disabilities in British Columbia. “It’s the model that’s broken and needs to be changed.”
Since the COVID-19 outbreak began, Adapt, another disability rights organization, has pushed for people to be immediately removed from nursing homes and other facilities during the pandemic. “Nursing homes are such deadly places. They always have been,” said Anita Cameron, an Adapt organizer in Rochester, New York. She cited a nursing facility for disabled children in New Jersey, where 11 kids died during an adenovirus outbreak in 2018. “You don’t hear the stories so much” in other times, Cameron said. “You’re just hearing it with COVID because it’s off the charts.”
The organization has called for the immediate passage of the Disability Integration Act, a bipartisan bill, first introduced in 2015, that aims to break down barriers to home- and community-based care options, including preventing insurers from denying coverage for such alternatives. “Right now a person who needs long-term services and support has a very limited choice where they can receive services,” said Senate Minority Leader Chuck Schumer of New York, when he introduced the latest version of the bill in January 2019.
Still, the bill has received no discussion since being referred to the Senate committee on health, education, labor, and pensions early in 2019.
While some disability rights activists have been vocal about envisioning a full transition to community care, aging rights advocates are often more hesitant to write off the nursing home model entirely. “Our messages are very, very similar: We need to look at alternatives to institutionalization,” said Patricia McGinnis, the founder and executive director of California Advocates for Nursing Home Reform, a consumer advocacy organization. But she also noted that some functions of nursing homes, including providing rehabilitation services for people after surgeries and providing 24-hour care, may be difficulty to replace fully with community-based models.
And experts and advocates agree that obstacles to deinstitutionalizing elder care abound. Cameron, the Adapt organizer, points out that it would be difficult to close nursing homes without offering more affordable housing options in the community. Another limiting factor is labor. Transition to home-based care would require more home health care workers—many of whom work for lower pay, and with fewer labor protections, than their counterparts in facilities. In some places, there are already too few people willing to fill those roles.
Elana Buch, a medical anthropologist at the University of Iowa who studies home health care, said advocates often argue that while community-based care for older adults would be less expensive than institutional care, “the whole system also relies on the idea that the workers will be poorly paid.”
In the past, these tensions have pitted unions and disability rights activists against each other, with labor representatives fighting to preserve the institutions that employ their members. There have been some attempts to bridge that divide, however, including a campaign called Caring Across Generations, launched in 2011 by Jobs With Justice and the National Domestic Workers Alliance, which advocates for more home care options for seniors—and better conditions for caregivers.
Still, even in countries that have pursued deinstitutionalization since the 1980s, such as Israel and Denmark—which, as Danish policy analyst Jon Kvist told Undark, has “the most encompassing free home care system in the world”—some people continue to end up in institutions, alongside robust options for community-based care.
In Denmark, at least, Kvist said, it’s currently difficult to tell whether the country’s pioneering elder care system necessarily helped reduce the impact of COVID And more generally, it remains unclear whether a transition to more home-based care would necessarily have protected against an infection like COVID-19, which has spread swiftly outside institutions, too. “Unfortunately, geriatrics as a field needs more research, more resources” in order to do “evaluation of safety in care provision outside of institutions,” said Mody, the Michigan infectious disease expert.
In the face of these obstacles, some health care workers have pushed for reforms that give people more choices as they age—and that make institutions seem less institutional. Barsness, the gerontology consultant, and others in the culture change movement have pushed for reforms would make nursing homes feel more welcoming and less hospital-like. McGinnis favors something closer to the model in Japan, where workers pay into a national long-term care insurance fund, which then funds a range of care options, with a strong emphasis on community care.
Many other advocates in the US have pushed for nursing homes that function more like resident-led intentional communities, or like small homes.
One national organization, the Green House Project, aims to replace large institutions with clusters of small homes, each housing around 10 to 12 residents, with private rooms and bathrooms and a shared, central kitchen and dining area. Susan Ryan, senior director at the Green House Project, told Undark that the organization has seen a surge in interest since the pandemic began.
Ryan said that, for years, they’ve received anecdotal reports that Green House homes seem to experience less influenza than large neighboring facilities. And, during COVID-19, she said, Green House homes have had few cases: The most recent internal tally, based on reports from 178 homes, found just 22 total COVID-19 cases, scattered among nine homes, and one death. The group is now working with a researcher at the University of North Carolina at Chapel Hill to collect data on infection spread.
The Green House model is unlikely to satisfy advocates who seek a full end to institutions of all kinds, including group homes. Ryan told Undark that she understands that perspective, because she used to hold it herself. As a nurse, she spent years working in nursing homes. She left in order to focus on home care, but ultimately returned to work within the nursing home model.
By way of explanation, Ryan told a personal story: Shortly before her mother died last year, she begged that the family keep Ryan’s stepfather, who had experienced significant cognitive loss, in his own home and out of an institution. In response, the family did manage to arrange and pay for the home care her stepfather needed, Ryan said, but he clashed with the health care aide, and seemed withdrawn and depressed. In the end, the family decided that he might be better served in a small institution, around other people.
“This is what drove me, in 2001, back into long-term care,” Ryan said. Not everyone, she argues, can afford round-the-clock home care and public funding is unlikely to close that gap soon. And, even if home care were universally available, she said, “I don’t know that we would address our need, as humans, for social connectedness, and to be connected to other people.”
For now, many nursing homes across the country remain on lockdown, and the industry is reeling from financial losses as staff demand hazard pay, costs for protective equipment and other materials mount, and would-be residents scramble for alternatives. “Our hearts are breaking over the completely disproportionate level of death in these facilities,” said Dooha, the New York City independent living advocate. “And we think there’s a lesson to be learned.”
By Michael Schulson | June 29, 2020
Source: Mother Jones






