
by Vikram Makhija | Feb 27, 2022 | Blog |
Most people think that they can just take care of an elderly parent or relative at home and don’t need to hire a home health agency. But this is actually not the case. Here are four reasons why you should hire a home health agency.
1) Home health agencies provide skilled nursing services. This includes monitoring vital signs, providing medication, wound care, and more.
2) They can also help with household tasks such as cooking, cleaning, and laundry.
3) Home health agencies provide social interaction and companionship for your loved one. This is especially important for those who may be isolated or lonely.

4) Lastly, home health agencies can help reduce the overall cost of caregiving. This is because they can provide services that you may not be able to do on your own.
5) You may need a home health agency if you’re recovering from surgery or an illness.
6) A home health agency can provide you with the necessary medical care and support to recover in the comfort of your own home.
7) Home health agencies offer a wide range of services, including nursing care, physical therapy, and social work services.
8) They can also provide important emotional support to help you through your recovery.
9) Home health agencies are often less expensive than staying in a hospital or nursing home.
10) They can also be more convenient, since the care and support is provided right in your own home.
11) You or a loved one is aging and needs more care than you can provide
12) You have a chronic illness that requires regular monitoring and care
13) You are recovering from an illness or surgery and need help with basic tasks
14) You are a busy working caregiver and need some respite time
15) Your loved one lives in a different city or state and you want them to be able to come home for visits
16) You want the peace of mind that comes with knowing someone is always there to help when needed
Hiring a home health agency is a great way to ensure that your loved one receives the care they need and deserve. They can provide skilled nursing care, assistance with household tasks, social interaction, and much more.
Home health agencies are also often less expensive than other forms of caregiving, such as nursing homes or hospitals. So if you’re looking for quality care for your loved one, consider hiring a home health agency.
Conclusion paragraph
So, if you are considering taking care of an elderly parent or relative at home, think again. The time and effort it will take to properly care for them is not something most people can manage on their own.
Home health agencies provide the necessary support and resources so that both the elderly person and their caregiver can be as comfortable and stress-free as possible.
If you are in need of these services, please reach out to us. We would be more than happy to discuss our services with you and answer any questions you may have.
by Vikram Makhija | Feb 23, 2022 | Blog |
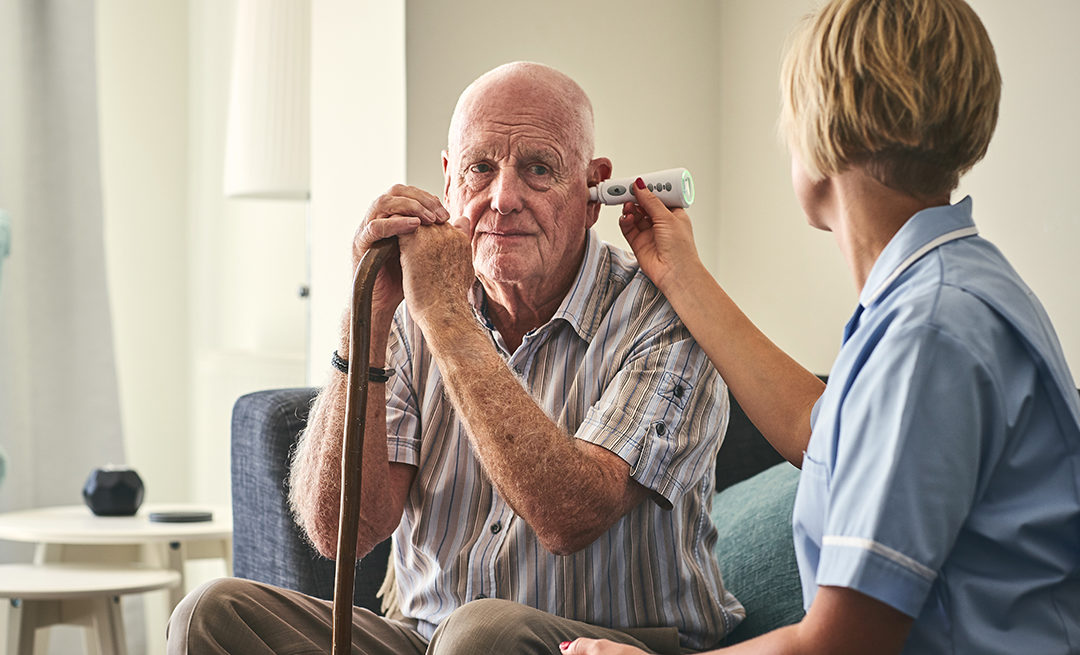
So you’re considering hiring a home care or home health service for a loved one – but what’s the difference? Home health services are licensed medical professionals, such as nurses and therapists, who provide healthcare services in the patient’s home.
Home care services usually include personal care assistance like bathing, dressing, and grooming, as well as light housekeeping and meal preparation. Here’s a breakdown of the services each type of agency typically offers:
Home health agencies will provide more comprehensive medical care including wound care, pain management, injections, and more. They may also offer skilled nursing visits and physical therapy.

Home care agencies generally do not offer medical services beyond personal care assistance. However, they can connect you with other resources in your community like meal delivery, transportation, and social programs.
Home health services are typically more expensive than home care services. In most cases, Medicare and Medicaid will cover home health services, but not home care.
If you’re not sure which type of service is right for your loved one, contact your local Area Agency on Aging for more information. They can help connect you with the right resources in your community.
Home health care and homecare services are often confused with one another. Though they do have some key differences, most people assume that these two types of offerings overlap when in reality there is very little resemblance between them at all!
Home Health Care provides medical supervision by professionals such as nurses or therapists while it’s counterparts – “personal caregiver” based assistance isn’t always licensed but can still provide great support for loved ones who need help caring throughout their lives no matter what condition they’re facingcurrently battling illness on top offulling down stairs.
In fact, home health care is a great option for those who are chronically ill, recovering from surgery, or have a disability. Home health aides can help with a wide range of tasks such as bathing, dressing, and grooming; managing medications; and providing moral support.
On the other hand, home care services are geared towards helping seniors live comfortably in their own homes by providing assistance with activities of daily living (ADLs) like bathing, dressing, and grooming. In most cases, home care workers do not provide medical services – though they may be able to connect you with other resources in your community. Home care is often less expensive than home health care and is typically covered by Medicare and Medicaid.
If you’re not sure which type of service is right for your loved one, contact your local Area Agency on Aging for more information. They can help connect you with the right resources in your community.
For more information on home health care and home care services, visit the website of the M&Y Care LLC.

by Vikram Makhija | Feb 20, 2022 | Blog |
Did you know that there are home care services near me in my area? You might be surprised to learn that there are many different types of home care services that can provide support for you or your loved ones.
Whether you’re looking for help with daily activities, personal care, or just need someone to check in on you, there is a service out there that will fit your needs. Let’s take a closer look at some of the best ways to find home care services near me in my area.
One of the best ways to find home care services near me is by checking online directories like Yelp or Google Maps. These directories have comprehensive lists of providers in your area, so you can easily compare and contrast Angie’s List Home Care Services .
Another great way to find home care services near me is by contacting your local Area Agency on Aging. These agencies can provide you with a list of providers in your area, as well as information about the different types of services that are available.

If you’re looking for a specific type of service, such as dementia care, it can be helpful to contact a national organization like the Alzheimer’s Association. This organization maintains a database of providers who offer specialized services, so you can find the best care for your loved one.
No matter how you choose to find home care services near me, it’s important to make sure that the provider is licensed and insured. You should also ask for references from past clients to ensure that you’re making the best decision for your loved one.
Finding home care services near me can be a daunting task, but it’s important to take the time to find the right provider. By using online directories, contacting local agencies, and contacting national organizations, you can quickly and easily find the best provider for your needs.
We hope you enjoyed our article on home care services! If you have any questions or comments, please feel free to leave them below. Thanks for reading!
Conclusion paragraph
If you’re looking for home care services, it’s important to do your research and find a provider that fits your needs. There are many different types of home care services available, so take the time to find one that best suits your needs. You can use the tips we’ve provided here to get started, or contact us for more help finding the right service for you.

by Vikram Makhija | Feb 15, 2022 | Blog |
All home care agencies should take measures to protect their clients. This includes implementing policies and procedures that prevent abuse, neglect, and exploitation from happening.
Quality agencies also have staff who are properly trained in how to identify and report any incidents that occur.
Having a safe environment for your loved ones is crucial, so be sure to do your research before selecting a home care agency. Look for one that has a good reputation and is licensed and insured.
If you are ever concerned about the safety of your loved one, don’t hesitate to reach out to the home care agency. They should be more than happy to address your concerns and take any necessary actions to ensure your loved one’s safety.

What to Look for in a Quality Home Care Agency
When looking for a quality home care agency, there are several things you should keep in mind.
First, it’s important to make sure the agency is licensed and insured. This will ensure that they are compliant with all state regulations and that they have liability insurance in case of any accidents.
You should also look for an agency with a good reputation. Ask your friends and family if they have any recommendations, or do a quick online search to see what other people are saying about the agency.
It’s also important to consider the staff at the agency. Are they properly trained and qualified? Do they seem caring and compassionate? It’s important to feel comfortable with the people who will be taking care of your loved one.
Make sure to ask the agency about their policies and procedures. How do they prevent abuse, neglect, and exploitation from happening? What steps do they take if an incident occurs? It’s important to feel confident that the agency is doing everything possible to keep your loved one safe.
What to look for in a home care agency infographic
If you’re looking for a quality home care agency for your loved one, be sure to keep the following in mind:
-The agency should be licensed and insured.
-They should have a good reputation.
-The staff should be qualified and compassionate.
-The agency should have policies and procedures in place to prevent abuse, neglect, and exploitation.
-You should feel confident that the agency is doing everything possible to keep your loved one safe.
How To Find The Right Home Care Services?
There are a few things to consider when looking for home care services. The first is what type of care you need. Home health aides can help with basic needs like bathing, dressing, and grooming, while nurses can provide more extensive medical care.
The second thing to consider is price and insurance coverage. Most home care services are not covered by insurance, so you’ll need to factor that into your budget.
The third thing to consider is the quality of the service. You’ll want to make sure you choose a reputable company with qualified staff who will meet your needs efficiently and effectively.
You can ask family and friends for recommendations or do online research to find the best fit for your needs.
What you need to know before hiring a home care agency?
Before hiring a home care agency, it’s important to do your research. You’ll want to ask around and get recommendations from friends and family, as well as look for online reviews.
You’ll also want to make sure the agency is licensed and insured, and that their caregivers are qualified and experienced. It’s also important to discuss your specific needs with the agency so they can match you with the best caregiver possible.
Lastly, be sure to have an agreement in place specifying the services the caregiver will provide, as well as how much it will cost. This will help avoid any misunderstandings down the road.
Ways to choose the best Home Care Agency for your loved ones
Here are a few tips to help you choose the best home care agency for your loved ones:
- Ask your friends and family members if they have any recommendations.
- Do some research online and read reviews from previous clients.
- Meet with the representatives from a few different agencies and ask them specific questions about their services.
- Make sure the agency is licensed and insured.
- Ask about the caregivers’ training and experience levels.
- Schedule a trial period to test out the agency’s services before making a commitment.
How to protect home care clients from abuse and exploitation?
There are a few things that can be done to help protect home care clients from abuse and exploitation.
First, it’s important for families to be aware of the signs of abuse and exploitation, which can include unexplained bruises or injuries, sudden changes in mood or behavior, refusing to see friends or family members, being withdrawn or isolated, and having new possessions that cannot be accounted for.
If you suspect that your loved one is being abused or exploited, it’s important to report it immediately. You can contact M&Y Care LLC in your area or the police.
There are also advocacy groups available that can provide support and assistance. Finally, it’s important to remember that abuse and exploitation are not always easy to spot, so don’t hesitate to ask for help if you have any concerns.
Conclusion paragraph
No one ever wants to think about the possibility of abuse, neglect, or exploitation happening to their loved ones. But the fact is that it can happen anywhere, even in a home care setting.
That’s why it’s so important to select a quality home care agency that takes measures to protect its clients. Staff at quality agencies are properly trained and know how to identify and report any incidents that occur.
If you are ever concerned about the safety of your loved ones, be sure to reach out to the agency and ask questions.
The most important thing is that you feel comfortable with the agency you choose and that your loved ones are safe and well taken care of.

by Vikram Makhija | Feb 8, 2022 | Blog |
Did you know that there are home care service and health services available at affordable prices? Many people don’t realize this, because they think that they have to go to a hospital or doctor’s office to receive these services.
However, there are many companies who offer these services in the comfort of your own home. This can be a great option for those who want to save money and do not want to leave their home.
If you are interested in receiving home care service or health services, be sure to do your research first. There are many different companies out there that offer these services, so it is important to find one that fits your needs.
You should also compare prices between different companies before making a decision. By doing this, you can be sure that you are getting the best deal possible.

If you are looking for home care service or health services, be sure to check out the companies below.
Some of the top companies that offer home care service and health services include:
- -Comfort Keepers
- -Home Instead Senior Care
- -Right at Home
Each of these companies offers a variety of services that can meet your needs. Be sure to research each company to find the one that is right for you.
If you are looking for affordable health services, be sure to check out the companies below.
Some of the top companies that offer affordable health services include:
- -M&Y Care LLC
- -Medi-Share
Each of these companies offers a variety of services that can meet your needs. Be sure to research each company to find the one that is right for you.
By choosing a company that offers home care service or health services, you can be sure that you are getting the best possible care. These companies offer quality services at an affordable price, so you can rest easy knowing that you are in good hands. Be sure to research the different companies available to find the one that is right for you.
Comparison of Home Health Aide Services
When looking for home health aide services, it’s important to compare your options. Not all agencies are created equal, and some may offer more comprehensive services than others.
The best way to determine what agency is right for you is to review their services and compare them to your needs.
Some of the things you’ll want to consider when comparing agencies include:
- The scope of services offered
- The quality of care provided
- The type of staff employed by the agency
- Registered nurses on staff
- How long the agency has been in business
- The size of the agency
Once you’ve considered all of these factors, you’ll be able to select the agency that is best for you and your loved one.
When looking for home health aide services, it’s important to compare your options. Not all agencies are created equal, and some may offer more comprehensive services than others.
The best way to determine what agency is right for you is to review their services and compare them to your needs.
Some of the things you’ll want to consider when comparing agencies include:
- The scope of services offered
- The quality of care provided
- The type of staff employed by the agency
- Registered nurses on staff
- How long the agency has been in business
Once you’ve considered all of these factors, you’ll be able to select the agency that is best for you and your loved one. A home health aide can provide many benefits to a senior, including:
- Help with Activities of Daily Living (ADLs)
- Meal Preparation
- Medication Management
- Escorting to Appointments
- Light Housekeeping
When considering home health aide services, it’s important to find an agency that offers the services that are most important to you and your loved one. Comparing agencies is the best way to find the one that fits your needs.
Some home health aides provide more comprehensive services than others. When comparing agencies, be sure to consider the scope of services offered as well as the quality of care provided.
You’ll also want to consider the type of staff employed by the agency and how long they have been in business. By comparing agencies, you’ll be able to find the one that is best for you and your loved one.
Conclusion paragraph
Home care service and health services are available at affordable prices. If you are interested in receiving these services, be sure to do your research first. There are many companies who offer these services, so it is important to find the right one for you. Thanks for reading!

by Vikram Makhija | Feb 1, 2022 | Blog |
A home care agency is a business that provides services to people in their homes. These services can include anything from bathing and dressing to cooking and cleaning.
Home care agencies are often used by the elderly, disabled, or those who are unable to leave their home for any reason. There are many different types of home care agencies, but all of them share one common goal: to protect their clients.
This can be done in many ways, but most often it involves ensuring that the client is safe and healthy at all times. Home care agencies strive to provide high-quality service so that their clients can live comfortably and safely in their own homes.
There are many benefits to using a home care agency. Perhaps the most important benefit is that it allows people to remain in their own homes, which is often where they feel most comfortable.

Home care agencies can also be cost-effective, especially when compared to other types of care such as nursing homes or assisted living facilities. In addition, home care agencies offer a high level of personalization, which is important for many seniors and disabled individuals.
If you are looking for a quality home care agency, be sure to do your research. There are many excellent agencies out there, but it is important to find one that meets your specific needs.
Ask around for recommendations, or do a quick online search to find reviews from past clients. Once you have found a few agencies that seem like a good fit, contact them to learn more about their services.
It is important to interview several agencies before making a decision, as this will help ensure that you find the best one for you or your loved one.
Choosing the right home care agency can be daunting, but it is worth it for the peace of mind it provides. When you choose an agency that puts your safety and well-being first, you can rest assured knowing that you are in good hands.
There are many different types of home care agencies, but all of them share one common goal: to protect their clients.
One way home care agencies protect their clients is by ensuring that they are safe and healthy at all times. This can be done in many ways, but most often it involves making sure that the client has access to proper medical care and that they are following all of the doctor’s orders.
Home care agencies also strive to provide high-quality service. This means that they employ well-trained staff who are dedicated to meeting the needs of their clients. In addition, they use state-of-the-art equipment and technology to help ensure that the client is getting the best possible care.
Another benefit of using a home care agency is that it is often cost-effective. This is especially true when compared to other types of care such as nursing homes or assisted living facilities.
Finally, home care agencies offer a high level of personalization. This is important for many seniors and disabled individuals who want to maintain their independence and dignity.
If you are looking for a quality home care agency, be sure to do your research. There are many excellent agencies out there, but it is important to find one that meets your specific needs.
At M&Y Care LLC, we take a special interest in protecting our clients. Our nurses and therapists are highly skilled and experienced professionals who go the extra mile to ensure that our clients receive the best possible care.
Whether it’s providing medication reminders or helping with basic tasks like bathing and dressing, we always put our clients’ safety first.
We understand how important it is for them to feel comfortable and safe in their own homes, and we work tirelessly to make sure that they get the quality care they need and deserve.
If you are interested in learning more about our services, please contact us today. We would be happy to answer any of your questions and discuss how we can help you or your loved one stay safe and comfortable at home.
There are many benefits to using a home care agency, including the ability to remain in your own home, cost-effectiveness, personalization, and more.
When choosing a home care agency, it is important to do your research to find one that meets your specific needs. M&Y Care LLC is a quality home care agency that puts your safety and well-being first.
Contact us today to learn more about our services. We would be happy to answer any of your questions.
A home care agency is a business that provides services to people in their homes. These services can include anything from bathing and dressing to cooking and cleaning. Home care agencies are often used by the elderly, disabled, or those who are unable to leave their home for any reason. There are many different types of home care agencies, but all of them share one common goal: to protect their clients. This can be done in many ways, but most often it involves ensuring that the client is safe and healthy at all times. Home care agencies strive to provide high-quality service so that their clients feel comfortable and safe in their own homes.












